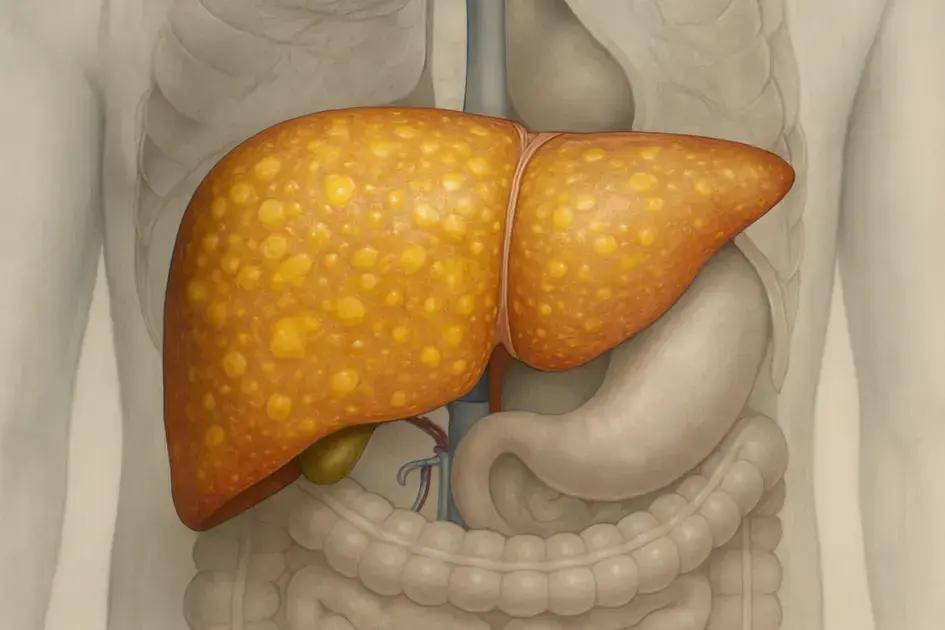
Fatty liver disease is a condition characterized by the accumulation of excess fat in the liver, which can lead to complications such as liver inflammation, cirrhosis, and cardiovascular issues; effective management involves lifestyle changes like a balanced diet, exercise, and weight control.
When we talk about fatty liver disease icd 10, it might sound complex, but it’s really important to understand what it implies for your health. So, have you ever wondered what this diagnosis entails and how it might affect you? Let’s dive into the details.
Overview of fatty liver disease
Fatty liver disease is a condition characterized by an excessive accumulation of fat in the liver. This condition can occur in individuals who consume little to no alcohol, known as non-alcoholic fatty liver disease (NAFLD). There are various forms of fatty liver disease, but the most common are simple fatty liver, which usually does not cause liver damage, and non-alcoholic steatohepatitis (NASH), which can lead to inflammation and liver cell damage.
Why Does Fatty Liver Disease Occur?
Fatty liver disease can develop due to several factors, including obesity, insulin resistance, and metabolic syndrome. When your body cannot properly metabolize fats, they can build up in the liver. Additionally, certain medications, rapid weight loss, and malnutrition can also contribute to this condition.
Symptoms of Fatty Liver Disease
Many people with fatty liver disease do not experience noticeable symptoms. However, some may suffer from fatigue, discomfort in the upper right abdomen, and unexplained weight loss. As the disease progresses, more serious issues may arise, such as liver inflammation or scarring.
Who is at Risk?
The risk factors for developing fatty liver disease include obesity, type 2 diabetes, high cholesterol, and high blood pressure. A sedentary lifestyle and poor dietary choices, such as a diet high in sugars and fats, can also increase the risk.
What is ICD 10?
ICD 10, or the International Classification of Diseases, 10th Revision, is a medical coding system used worldwide to standardize the classification of diseases and health conditions. Developed by the World Health Organization (WHO), it provides codes for diseases, signs, symptoms, abnormal findings, complaints, social circumstances, and external causes of injury or disease.
Purpose of ICD 10
The main purpose of ICD 10 is to facilitate the collection, analysis, and comparison of health information across countries. This coding system aids healthcare providers, insurance companies, and researchers in understanding health trends and making informed decisions.
ICD 10 Structure
ICD 10 codes are alphanumeric and consist of up to seven characters. The first character is a letter, followed by numbers that further specify the condition. For example, the code for fatty liver disease is K76.0, where K represents a diagnosis related to the liver.
Impact on Healthcare
ICD 10 has improved clinical documentation and coding practices. Accurate coding can lead to better treatment options, improved reimbursement for healthcare providers, and enhanced patient care. It has also made medical data more accessible for research and public health initiatives.
Symptoms of fatty liver disease
Many people with fatty liver disease do not experience noticeable symptoms in the early stages. However, as the disease progresses, some common symptoms may begin to appear.
Common Symptoms
Individuals may experience fatigue, which can be subtle at first but may become more pronounced as the disease progresses. Another symptom is discomfort or a sense of fullness in the upper right abdomen, near the liver.
Additional Symptoms
Some people may also notice unexplained weight loss or mild pain in the liver area. In more severe cases, symptoms like jaundice, which is a yellowing of the skin and eyes, may occur due to liver dysfunction. This is a sign of advanced liver disease requiring immediate medical attention.
When to Seek Medical Help
If you experience persistent fatigue, abdominal discomfort, or any signs of jaundice, it is important to consult a healthcare provider. Early diagnosis and management of fatty liver disease can prevent severe liver problems.
Risk factors of fatty liver disease

Understanding the risk factors of fatty liver disease is essential for prevention and early detection. Several factors can increase the likelihood of developing this condition, and being aware of them can help individuals make informed health choices.
Obesity
Obesity is one of the primary risk factors. Excess body weight, particularly around the abdomen, can lead to fat accumulation in the liver. Losing weight through a balanced diet and regular exercise may significantly reduce the risk.
Type 2 Diabetes
Type 2 diabetes is another significant risk factor. Insulin resistance, common in individuals with diabetes, can contribute to fat buildup in the liver. Proper management of blood sugar levels is crucial for those at risk.
High Cholesterol and Triglycerides
Having high cholesterol and elevated triglyceride levels can also lead to fatty liver disease. A diet low in saturated fats and sugars, along with regular exercise, can help maintain healthy cholesterol levels.
Sedentary Lifestyle
A sedentary lifestyle contributes to various health issues, including fatty liver disease. Regular physical activity plays a vital role in managing weight and improving liver health.
Poor Diet
A diet high in sugars, refined carbohydrates, and unhealthy fats can increase the risk of developing fatty liver disease. Incorporating more whole foods, vegetables, and lean proteins can positively impact liver health.
Age and Gender
Age can also be a factor; individuals over 50 may have a higher risk. Additionally, studies suggest that men are more likely to develop fatty liver disease than women.
Diagnosis of fatty liver disease
The diagnosis of fatty liver disease typically involves several steps to accurately identify the condition and assess its severity. Physicians may rely on a combination of medical history, physical exams, and various tests to confirm the diagnosis.
Medical History
First, your doctor will ask about your medical history, including any symptoms you may have experienced, such as fatigue or abdominal discomfort. They will also inquire about your lifestyle, including alcohol consumption, diet, and physical activity levels, as these can influence liver health.
Physical Examination
During the physical exam, the doctor may check for signs of liver disease, such as swelling in the abdomen or jaundice, which is a yellowing of the skin and eyes. This assessment helps to understand how the liver is functioning.
Blood Tests
Blood tests are crucial in the diagnosis of fatty liver disease. These tests can measure liver enzymes, which may be elevated if the liver is damaged. Common tests include alanine aminotransferase (ALT) and aspartate aminotransferase (AST). High levels of these enzymes can suggest liver inflammation.
Imaging Tests
If blood tests indicate fat accumulation or liver inflammation, the physician may recommend imaging tests. Ultrasound is often the first test performed as it is non-invasive and can effectively detect fat in the liver. Other imaging techniques, such as CT scans or MRIs, can provide more detailed views of the liver.
Liver Biopsy
In some cases, a liver biopsy may be necessary to confirm the diagnosis and to assess the degree of liver damage. This procedure involves taking a small sample of liver tissue for examination under a microscope. This is often performed if there are concerns about potential liver damage or scarring.
ICD 10 codes for fatty liver
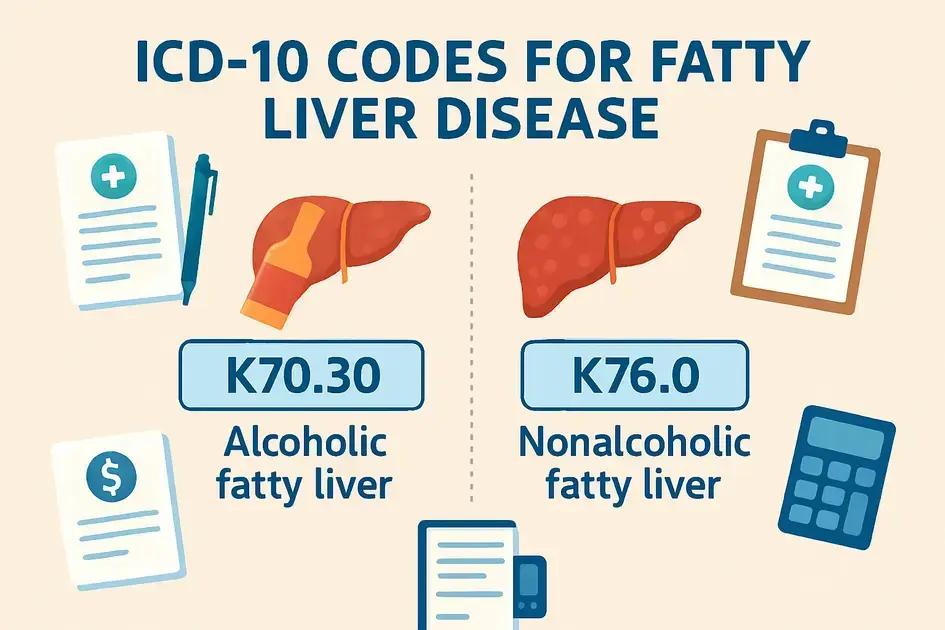
ICD 10 codes are essential for classifying diseases and health conditions, including fatty liver disease. These codes allow healthcare providers and insurers to accurately document and track the prevalence and management of liver conditions.
Specific ICD 10 Codes
The primary ICD 10 code for fatty liver disease is K76.0, which refers specifically to hepatic steatosis, commonly known as fatty liver. This code encompasses both alcoholic and non-alcoholic cases. It is important for medical professionals to choose the correct code for accurate billing and treatment records.
Distinguishing Between Alcoholic and Non-Alcoholic Fatty Liver
For better specificity, different codes are used to classify alcoholic and non-alcoholic fatty liver disease. For instance:
- K70.0 refers to alcoholic fatty liver disease.
- K76.0 refers to non-alcoholic fatty liver disease.
Understanding and using the right ICD 10 codes is critical in many aspects, including clinical studies, epidemiological tracking, and healthcare planning.
Importance of Accurate Coding
Accurate coding helps ensure that patients receive appropriate care and that healthcare providers are reimbursed correctly. Moreover, it contributes to broader research and public health efforts aimed at understanding and reducing the impact of fatty liver disease.
Treatment options for fatty liver disease
Treatment options for fatty liver disease largely depend on the cause and severity of the condition. In many cases, lifestyle changes can significantly improve liver health and prevent further damage.
Lifestyle Changes
Weight loss is one of the most effective strategies for treating fatty liver disease, especially in individuals who are overweight or obese. Losing even 5-10% of body weight can reduce liver fat and improve liver function.
Dietary Adjustments
Adopting a healthy diet is crucial. Focus on consuming a balanced diet rich in fruits, vegetables, whole grains, and lean proteins. Reducing the intake of sugar, refined carbohydrates, and saturated fats can provide significant benefits. Foods high in omega-3 fatty acids, such as fish, can also help.
Exercise
Engaging in regular physical activity is important for improving liver health. Aim for at least 150 minutes of moderate exercise each week. Activities can include walking, swimming, or cycling, which help burn calories and reduce liver fat.
Medications
While there are currently no specific medications approved for fatty liver disease, some may be prescribed to manage related conditions. For instance, medications to control diabetes, cholesterol, and triglycerides may help address underlying factors contributing to the disease.
Monitoring and Follow-Up
Regular follow-up appointments with your healthcare provider are essential to monitor liver health and adjust treatment plans as needed. Blood tests and imaging studies may be used to assess the effectiveness of the treatment.
Lifestyle changes for liver health

Making lifestyle changes is crucial for improving liver health, especially for those dealing with fatty liver disease. Simple adjustments can lead to significant improvements in liver function and overall well-being.
Healthy Diet
A balanced diet is essential for liver health. Focus on consuming a variety of fruits, vegetables, whole grains, and lean proteins. Avoid processed foods, sugary snacks, and excess carbohydrates. Including foods rich in omega-3 fatty acids, such as fish, can help reduce fat in the liver.
Weight Management
Achieving and maintaining a healthy weight is vital. For those who are overweight or obese, losing just 5-10% of body weight can lead to improvements in liver health. Combining a healthy diet with regular exercise can facilitate weight loss.
Regular Physical Activity
Engaging in exercise is another key factor. Aim for at least 150 minutes of moderate-intensity aerobic activity each week. Activities like walking, swimming, or cycling help improve liver function and assist in weight management.
Avoid Alcohol
Limiting or completely avoiding alcohol consumption is critical for liver health. Alcohol can cause further damage to the liver, particularly in individuals with fatty liver disease. If you drink, do so in moderation and consider discussing it with your healthcare provider.
Stay Hydrated
Drinking plenty of water is important. Staying hydrated helps the liver function properly and supports metabolic processes. Aim for at least 8 glasses of water a day, or more if you are physically active.
Regular Check-ups
Lastly, regular check-ups with a healthcare provider are essential. These appointments can help monitor liver health and catch any potential issues early.
Dietary recommendations for fatty liver disease
Dietary recommendations play a critical role in managing fatty liver disease. Making wise food choices can help reduce liver fat and improve overall liver health.
Focus on Whole Foods
Incorporate more whole foods into your diet. Foods like fruits, vegetables, whole grains, and legumes provide essential nutrients without added sugars and unhealthy fats. Aim for at least five servings of fruits and vegetables each day.
Limit Sugar and Saturated Fats
Reducing your intake of sugar and saturated fats is crucial. Avoid sugary drinks, candies, and desserts. Instead, choose healthier alternatives like unsweetened beverages and natural sweeteners, when necessary.
Include Healthy Fats
Healthy fats, such as those found in avocados, nuts, seeds, and fatty fish, can support liver health. Incorporating omega-3 fatty acids is particularly beneficial. Aim to include foods like salmon, walnuts, and flaxseeds in your diet.
Opt for Lean Proteins
Choose lean sources of protein, such as chicken, turkey, beans, tofu, and fish. These options provide the necessary nutrients without adding extra fat that can contribute to liver issues.
Stay Hydrated
Drinking enough water is vital for liver function. Aim to consume at least 8 cups of water daily. Staying hydrated helps the liver process nutrients and eliminate toxins more efficiently.
Be Mindful of Portion Sizes
Controlling portion sizes can help prevent overeating. Using smaller plates and paying attention to hunger cues can aid in maintaining a healthy weight and improving liver health.
Role of exercise in managing fatty liver

Exercise plays a vital role in managing fatty liver disease. Regular physical activity can help reduce liver fat, improve overall liver function, and support weight management.
Weight Loss Benefits
One of the primary benefits of exercise is weight loss. Losing even a small percentage of body weight can lead to a significant reduction in liver fat. Combining cardiovascular exercises, such as walking, running, or cycling, with strength training can enhance weight loss efforts.
Improved Insulin Sensitivity
Regular physical activity can improve insulin sensitivity. This means that your body is better able to use insulin effectively, which can help prevent fat accumulation in the liver. Exercise helps regulate blood sugar levels, which is crucial for individuals with fatty liver disease.
Increased Metabolism
Exercise boosts metabolism, allowing the body to burn more calories even at rest. An increased metabolic rate can further assist in weight loss and help reduce liver fat.
Types of Recommended Exercises
A combination of aerobic and anaerobic exercises is often best. Aim for at least 150 minutes of moderate-intensity aerobic exercise each week. Activities like brisk walking, swimming, or cycling are effective. Additionally, include strength training at least two days a week to build muscle.
Consistency is Key
Consistency in exercising is crucial for managing fatty liver disease. Making exercise a regular part of your daily routine helps maintain liver health and overall well-being. Setting achievable goals and finding activities you enjoy can make it easier to stick with a routine.
Prevention strategies for fatty liver disease
Preventing fatty liver disease requires a proactive approach that includes lifestyle modifications and regular health monitoring. These strategies can help to reduce the risk of developing this condition.
Maintain a Healthy Weight
One of the most effective prevention strategies is to maintain a healthy weight. Being overweight increases the risk of fatty liver disease. Aim for a balanced diet and regular physical activity to help manage your weight effectively.
Follow a Balanced Diet
Adopting a balanced diet rich in whole foods, fruits, vegetables, lean proteins, and whole grains can support liver health. Avoid foods high in refined sugars, unhealthy fats, and processed ingredients to lower your risk.
Regular Exercise
Incorporating regular exercise into your routine can help prevent fatty liver disease. Aim for at least 150 minutes of moderate aerobic activity each week, such as brisk walking, swimming, or cycling, as well as strength training twice a week.
Limit Alcohol Consumption
Limiting or avoiding alcohol consumption is essential. Alcohol can damage liver cells and exacerbate liver problems. If you drink, do so in moderation and consult with a healthcare provider for guidelines.
Routine Medical Check-ups
Regular medical check-ups are crucial for monitoring liver health, particularly for those at risk. Routine blood tests can help identify liver function issues early, allowing for timely intervention.
Control Blood Sugar and Cholesterol Levels
Keeping blood sugar and cholesterol levels in check is vital. If you have diabetes, manage your condition carefully to prevent further complications. Following a healthy diet and regular exercise can help maintain these levels.
Complications associated with fatty liver
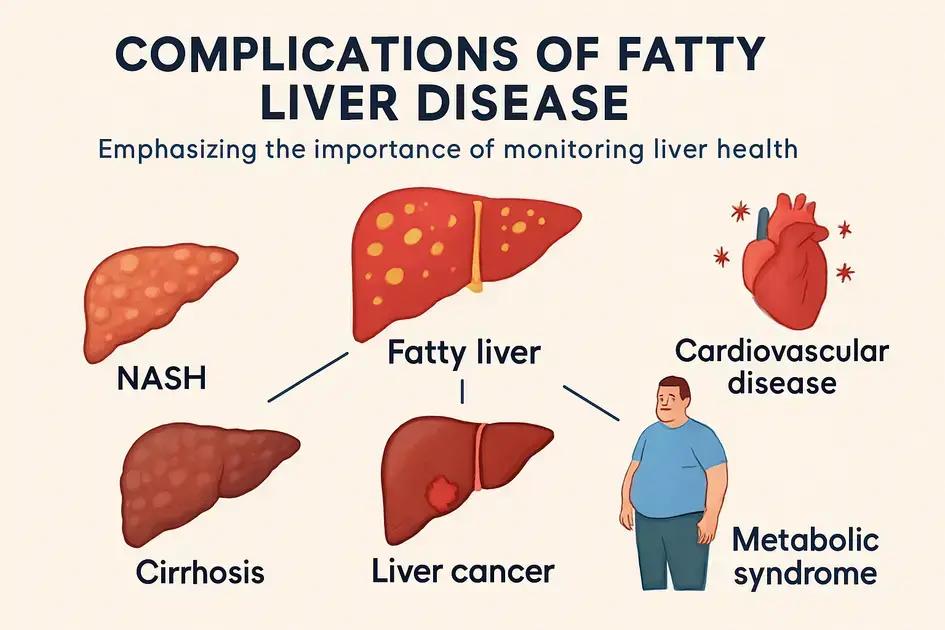
Fatty liver disease, if left untreated, can lead to several serious complications. Understanding these complications is essential for managing and preventing the progression of the disease.
Non-Alcoholic Steatohepatitis (NASH)
One potential complication is the progression to non-alcoholic steatohepatitis (NASH). This condition involves inflammation of the liver, which can lead to scarring and permanent liver damage. NASH is a more severe form of fatty liver disease and significantly increases the risk of liver complications.
Liver Cirrhosis
If NASH progresses, it can result in cirrhosis, which is the scarring of the liver tissue. Cirrhosis can impair liver function and lead to complications like liver failure. Individuals with cirrhosis may need a liver transplant to survive.
Increased Risk of Liver Cancer
People with fatty liver disease, especially those with cirrhosis, are at a higher risk of developing liver cancer. Regular monitoring and liver health assessments are necessary to catch any early signs of liver cancer.
Cardiovascular Disease
Research suggests a link between fatty liver disease and an increased risk of cardiovascular disease. Individuals with fatty liver may develop heart problems, including heart attack and stroke, due to associated conditions like high blood pressure and diabetes.
Metabolic Syndrome
Fatty liver disease is often associated with metabolic syndrome, a cluster of conditions that increase the risk of heart disease and diabetes. Components of metabolic syndrome include obesity, insulin resistance, high cholesterol, and high blood pressure.
Frequently asked questions about fatty liver disease
Addressing frequently asked questions (FAQs) about fatty liver disease can help individuals understand more about this condition and how to manage it effectively.
What is fatty liver disease?
Fatty liver disease is a condition where excess fat builds up in the liver. It can occur in people who drink little or no alcohol, known as non-alcoholic fatty liver disease (NAFLD), or in those who consume alcohol, known as alcoholic fatty liver disease.
What are the symptoms of fatty liver disease?
Many people with fatty liver disease do not experience noticeable symptoms. However, some may have fatigue, discomfort in the upper right abdomen, or an enlarged liver. In advanced cases, symptoms can progress to jaundice and severe abdominal pain.
What causes fatty liver disease?
Causes of fatty liver disease include obesity, insulin resistance, high blood sugar, high cholesterol, and excessive alcohol consumption. Other factors such as poor diet and sedentary lifestyle also contribute to the risk.
How is fatty liver disease diagnosed?
Diagnosis often involves a combination of medical history, physical examination, blood tests to check liver function, and imaging tests like ultrasound. In some cases, a liver biopsy may be performed for further evaluation.
Can fatty liver disease be reversed?
Yes, fatty liver disease can often be reversed with lifestyle changes. Maintaining a healthy weight, following a balanced diet, exercising regularly, and avoiding alcohol can reduce liver fat and improve liver health.
Is fatty liver disease serious?
While fatty liver disease itself may start as a benign condition, it can lead to serious complications such as non-alcoholic steatohepatitis (NASH), cirrhosis, and liver failure if not properly managed. Early intervention is critical.
Current research on fatty liver disease
Current research on fatty liver disease focuses on understanding its causes, progression, and potential treatments. This research is crucial for improving patient outcomes and developing effective management strategies.
Understanding the Disease Mechanisms
Researchers are working to uncover the biological mechanisms that lead to fat buildup in the liver. Studies are examining how factors like obesity, insulin resistance, and genetics contribute to the development of fatty liver disease and its progression to more severe forms, such as non-alcoholic steatohepatitis (NASH).
Longitudinal Studies
Longitudinal studies are being conducted to track patients over time, providing valuable insights into how fatty liver disease progresses and identifying risk factors associated with disease advancement. These studies help identify which individuals are most likely to develop serious complications.
Potential Treatment Options
Research is ongoing into various treatment options, including medications, dietary changes, and exercise interventions. Clinical trials are exploring the efficacy of drugs that target the underlying mechanisms of fatty liver disease, focusing on reducing liver fat and inflammation.
Impact of Lifestyle Interventions
Studies are being conducted to assess the impact of lifestyle changes, such as diet and physical activity, on fatty liver disease. These studies aim to establish clear guidelines for effective weight loss strategies and dietary modifications that can benefit liver health.
Emerging Technologies
New technologies, such as imaging techniques and biomarker discovery, are being developed to improve the diagnosis and monitoring of fatty liver disease. These advancements may lead to earlier detection and better assessment of liver fat levels and inflammation.
Support and resources for patients
Accessing the right support and resources is crucial for patients dealing with fatty liver disease. These resources can provide valuable information, counseling, and community support to help individuals manage their condition effectively.
Healthcare Providers
Consulting with healthcare providers is essential for any patient with fatty liver disease. Physicians, hepatologists, and dietitians can offer guidance, treatment options, and personalized plans to improve liver health. Regular check-ups can help monitor the disease’s progression and manage related health issues.
Patient Support Groups
Joining patient support groups can be beneficial for emotional well-being. These groups provide a platform for individuals to share experiences, challenges, and tips on managing fatty liver disease. Connecting with others facing similar issues can reduce feelings of isolation.
Educational Resources
Several organizations offer educational resources tailored to fatty liver disease. Websites like the American Liver Foundation provide articles, webinars, and links to research studies. These resources help patients understand their condition better and stay informed about the latest developments.
Nutritional Guidance
Access to a nutritionist or dietitian who specializes in liver health can be invaluable. They can create individualized meal plans that focus on nutrient-rich foods, which can help manage and improve liver function.
Online Communities and Forums
Participating in online forums and communities is another way for patients to seek support. These platforms allow individuals to ask questions, share experiences, and find tips on managing daily life with fatty liver disease.
In Conclusion: Managing Fatty Liver Disease
Understanding fatty liver disease is crucial for maintaining liver health and overall well-being. With the right lifestyle changes, such as a balanced diet and regular exercise, many people can effectively manage this condition.
Access to information and support resources can empower patients to take control of their health. From healthcare providers to patient support groups, each resource plays a vital role in helping individuals manage their condition.
Staying informed about current research and treatment options can also make a difference. By being proactive, patients can significantly reduce their risk of serious health problems associated with fatty liver disease.
Ultimately, with the right knowledge and tools, patients can lead healthier lives and prevent the progression of fatty liver disease.
FAQ – Frequently Asked Questions about Fatty Liver Disease
What is fatty liver disease?
Fatty liver disease is a condition characterized by the accumulation of excess fat in the liver, which can occur due to various factors like obesity, diabetes, and excessive alcohol consumption.
What are the main symptoms of fatty liver disease?
Many people with fatty liver disease experience no symptoms. However, some may notice fatigue, discomfort in the upper right abdomen, or mild pain.
How can I manage fatty liver disease effectively?
Managing fatty liver disease can be achieved through lifestyle changes such as maintaining a healthy weight, eating a balanced diet, engaging in regular exercise, and avoiding alcohol.
What lifestyle changes are recommended for liver health?
It’s recommended to follow a balanced diet rich in whole foods, exercise regularly, limit sugar and saturated fats, and stay hydrated to support liver health.
Are there support resources available for patients with fatty liver disease?
Yes, patients can access support through healthcare providers, patient support groups, educational resources, and online communities that focus on liver health.
Can fatty liver disease be reversed?
Yes, with appropriate lifestyle changes, many individuals can reverse fatty liver disease and improve their liver health significantly.