Living with diabetes involves managing symptoms through regular monitoring, healthy lifestyle choices, and understanding potential complications, emphasizing the importance of education and support in maintaining overall health.
Diabetes symptoms can be quite subtle at first, often making it hard to detect the condition early. Have you noticed any unusual signs in yourself or loved ones? In this article, we will dive into what to look for and the best ways to manage these symptoms.
Understanding diabetes: types and causes
Understanding diabetes is crucial for recognizing symptoms and managing the condition effectively. There are primarily three types of diabetes: type 1, type 2, and gestational diabetes. Each type has different causes and affects the body in unique ways.
Type 1 Diabetes
Type 1 diabetes occurs when the immune system mistakenly attacks insulin-producing cells in the pancreas. This results in little or no insulin being made. Individuals with type 1 diabetes often develop the condition during childhood or adolescence, although it can appear at any age.
Type 2 Diabetes
Type 2 diabetes is the most common form and usually develops when the body becomes resistant to insulin or when the pancreas fails to produce enough insulin. It often relates to lifestyle factors such as poor diet, lack of exercise, and being overweight. Unlike type 1, type 2 diabetes can develop gradually and is more common in adults.
Gestational Diabetes
Gestational diabetes occurs during pregnancy and is usually temporary, disappearing after giving birth. Nonetheless, it can pose risks to both mother and baby if not managed properly. Women who experience gestational diabetes are at a higher risk of developing type 2 diabetes later in life.
Common Causes of Diabetes
The exact cause of diabetes depends on the type, but common factors include genetics, lifestyle choices, and environmental influences. A family history of diabetes, unhealthy eating habits, physical inactivity, and obesity are significant risk factors.
Recognizing the early signs and understanding the different types of diabetes can help in seeking timely medical advice and managing health effectively.
Common early symptoms of diabetes

Recognizing common early symptoms of diabetes is vital for early diagnosis and management. Many people may not realize they have diabetes until symptoms become more severe. Here are some signs to watch for:
Increased Thirst
One of the first noticeable symptoms is often increased thirst. This occurs because the body is trying to remove excess sugar from the blood by drawing fluid from tissues, triggering thirst.
Frequent Urination
Along with thirst, many experience frequent urination. As your kidneys work harder to filter and absorb the excess sugar, more fluid is expelled, resulting in more trips to the bathroom.
Fatigue
Feeling unusually tired? Fatigue is another common early symptom because the body is unable to use glucose for energy properly, leading to feelings of tiredness and weakness.
Blurred Vision
Changes in fluid levels in the eye can cause blurred vision. As blood sugar levels rise and fall, vision may become less clear, making it harder to focus.
Increased Hunger
Experiencing an insatiable appetite? This could be due to increased hunger, as the body’s cells are unable to access glucose for energy, resulting in persistent feelings of hunger.
Unexplained Weight Loss
Unintended weight loss can occur as the body starts breaking down fat and muscle for energy when it cannot use glucose effectively.
Slow Healing Sores or Frequent Infections
High blood sugar levels can impact healing, leading to slow healing sores and an increased risk of infections, particularly skin infections or urinary tract infections.
Numbness or Tingling in Hands or Feet
Another red flag is numbness or tingling in the extremities, a condition known as neuropathy, which can result from prolonged high blood sugar levels.
If you or someone you know is experiencing these symptoms, it is essential to consult a healthcare professional for evaluation and guidance. Early detection can significantly impact the outcome of diabetes management.
What is type 1 diabetes?
Type 1 diabetes is a chronic condition where the pancreas produces little or no insulin. Insulin is a hormone that helps glucose enter the body’s cells for energy. Without enough insulin, glucose builds up in the bloodstream, leading to high blood sugar levels.
Causes of Type 1 Diabetes
While the exact cause is not fully understood, it is believed that an autoimmune reaction triggers type 1 diabetes. The body’s immune system mistakenly attacks and destroys insulin-producing cells in the pancreas. Genetic factors may also play a role in the development of this condition.
Who is Affected?
Type 1 diabetes can occur at any age, but it most commonly appears during childhood or adolescence. It affects both children and adults, and its symptoms can develop rapidly. Early diagnosis is crucial to manage the condition effectively.
Symptoms of Type 1 Diabetes
Common symptoms of type 1 diabetes include increased thirst, frequent urination, extreme hunger, unexplained weight loss, fatigue, and blurred vision. If these symptoms occur, it’s essential to seek medical attention.
Treatment and Management
Currently, there is no cure for type 1 diabetes. However, insulin therapy is used to manage blood sugar levels. People with type 1 diabetes must regularly monitor their blood glucose and adjust their insulin doses as needed. A balanced diet and regular physical activity also play important roles in managing the condition.
Living with Type 1 Diabetes
Living with type 1 diabetes requires commitment and education. Individuals must learn how to monitor their blood sugar levels and understand the impact of food and exercise on their health. Support from healthcare teams, family, and friends can make a significant difference.
Identifying type 2 diabetes symptoms

Identifying type 2 diabetes symptoms is essential for early diagnosis and effective management. Unlike type 1 diabetes, type 2 diabetes often develops slowly, and symptoms can sometimes be overlooked. Here are some common signs to watch for:
Increased Thirst and Frequent Urination
Many people with type 2 diabetes experience increased thirst and need to urinate more often. This happens because the kidneys work harder to filter excess glucose from the blood, leading to dehydration.
Extreme Fatigue
Fatigue is another common symptom. When the body cannot use insulin effectively, it cannot convert glucose into energy, leading to feelings of tiredness and low energy.
Blurred Vision
Changes in blood sugar levels can cause blurred vision. High glucose levels affect the eye’s lens, making it more difficult to focus. This symptom should not be ignored, as it can worsen over time.
Slow Healing of Cuts and Wounds
People with type 2 diabetes may find that cuts and wounds heal more slowly. High blood sugar can impair blood circulation and the body’s ability to heal, leading to persistent skin issues.
Dark Patches of Skin
Look out for dark patches of skin, especially in the folds and creases, such as the neck or armpits. This condition, called acanthosis nigricans, can be a sign of insulin resistance.
Increased Hunger
Despite eating, individuals with type 2 diabetes may feel increased hunger due to the body’s inability to effectively use glucose for energy. This can lead to frequent snacking and weight gain.
Numbness or Tingling Sensation
Some people experience numbness or tingling in their hands or feet, which can be a sign of nerve damage related to prolonged high blood sugar levels.
Frequent Infections
Type 2 diabetes can weaken the immune system, making individuals more susceptible to infections. If you notice recurrent skin infections or other infections, it’s essential to seek medical advice.
Recognizing these symptoms early can lead to timely intervention and better management of type 2 diabetes. It is important to consult a healthcare provider if you suspect any of these signs.
Gestational diabetes: what to know
Gestational diabetes is a type of diabetes that develops during pregnancy and typically disappears after giving birth. However, it can pose risks for both the mother and the baby, making it essential to understand the condition.
Causes of Gestational Diabetes
During pregnancy, hormonal changes can affect how insulin works in the body. Increased insulin resistance can lead to elevated blood sugar levels. Factors contributing to gestational diabetes include obesity, family history of diabetes, and certain ethnic backgrounds.
Risk Factors
Several risk factors can increase the likelihood of developing gestational diabetes. These include being over the age of 25, having a history of gestational diabetes in previous pregnancies, and having polycystic ovary syndrome (PCOS). Additionally, not being physically active can contribute to the risk.
Symptoms
Many women do not experience noticeable symptoms of gestational diabetes. However, some may notice increased thirst, fatigue, frequent urination, or blurred vision. Regular screening during pregnancy can help identify the condition even if symptoms are absent.
Managing Gestational Diabetes
Managing gestational diabetes typically involves monitoring blood sugar levels, following a healthy eating plan, and engaging in regular physical activity. In some cases, insulin therapy may be needed to control blood sugar levels effectively.
Importance of Monitoring
Frequent monitoring is crucial, as uncontrolled gestational diabetes can lead to complications for both the mother and the baby. Risks include having a larger baby, which may lead to delivery complications, and increased chances of developing type 2 diabetes later in life.
Postpartum Considerations
After giving birth, it’s important to have blood sugar levels checked to ensure they return to normal. Many women with gestational diabetes are at a higher risk for developing type 2 diabetes in the future, making follow-up care essential.
How high blood sugar affects the body
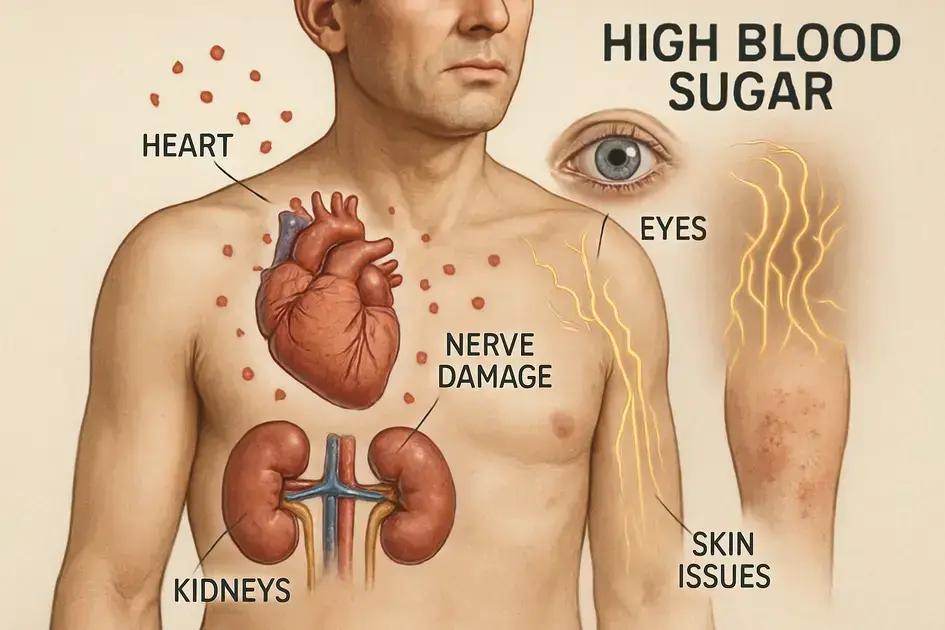
High blood sugar, also known as hyperglycemia, occurs when there is too much glucose in the bloodstream. This condition can significantly affect various parts of the body and lead to serious health issues if not managed properly.
Impact on Blood Vessels
Elevated blood sugar levels can damage blood vessels over time. This affects circulation and can lead to complications such as heart disease and stroke. Poor blood flow can also result in numbness or tingling in the extremities.
Effects on the Kidneys
High blood sugar can stress the kidneys, which filter waste from the blood. Over time, this can lead to a condition called diabetic nephropathy, where the kidneys become less effective. Serious cases may even result in kidney failure, requiring dialysis or a kidney transplant.
Nerve Damage
Extended periods of high blood sugar can lead to neuropathy, or nerve damage. This can result in pain, tingling, or loss of sensation, especially in the hands and feet. Diabetic neuropathy can affect daily activities and overall quality of life.
Vision Problems
High glucose levels can cause fluid to leak into the eye’s lens, leading to blurred vision and other vision issues. If left untreated, it can progress to diabetic retinopathy, a serious condition that can result in blindness.
Skin Issues
People with high blood sugar may experience a variety of skin problems, including dry skin and infections. High blood sugar can also lead to the formation of sores that heal slowly, increasing the risk of infection.
Weight Changes
Managing high blood sugar can sometimes lead to weight changes. While some may gain weight due to insulin resistance, others may experience weight loss if the body starts breaking down fat for energy instead of glucose.
Gastrointestinal Issues
High blood sugar can affect the nerves controlling the digestive system, leading to gastrointestinal issues like gastroparesis, where food moves slower through the stomach. This can cause bloating, nausea, and constipation.
Managing diabetes symptoms effectively
Managing diabetes symptoms effectively involves a combination of lifestyle changes, medication, and regular monitoring. Each individual may have different needs, so it’s essential to tailor a management plan that works best for you.
Monitoring Blood Sugar Levels
Regularly monitoring blood sugar levels is crucial for anyone with diabetes. Using a glucose meter, individuals can track their blood sugar throughout the day. This helps in understanding how food, activity, and medication affect glucose levels.
Healthy Eating
Adopting a balanced diet is key to managing diabetes symptoms. Focus on whole foods, such as fruits, vegetables, whole grains, lean proteins, and healthy fats. It’s also important to watch portion sizes and limit high-sugar and high-fat foods.
Physical Activity
Engaging in regular physical activity can help maintain a healthy weight and improve insulin sensitivity. Aim for at least 150 minutes of moderate exercise each week, including activities you enjoy, such as walking, swimming, or cycling.
Medication Management
For some individuals, taking medication is necessary to control blood sugar levels. This can include insulin or oral medications. It’s important to follow a healthcare provider’s instructions and communicate any side effects experienced.
Managing Stress
Stress management is often overlooked but is vital for managing diabetes. High stress can lead to elevated blood sugar levels. Techniques such as mindfulness, yoga, and deep breathing can help reduce stress.
Getting Regular Health Check-ups
Regular check-ups with healthcare providers are essential. These visits allow for monitoring of diabetes-related complications and adjustments to treatment plans if necessary. Discuss any new symptoms or concerns during these appointments.
Support Networks
Building a support network of family and friends can help in managing diabetes. Connecting with support groups or diabetes educators can offer practical advice and emotional support, making the journey easier.
Dietary tips for symptom management

Managing diabetes symptoms effectively often requires careful attention to dietary choices. Eating the right foods can help maintain stable blood sugar levels and improve overall health. Here are some essential dietary tips for symptom management:
Focus on Whole Foods
Incorporate whole foods into your diet. Foods such as fruits, vegetables, whole grains, lean proteins, and healthy fats provide essential nutrients without added sugars. These foods can help keep blood sugar levels steady.
Control Portion Sizes
Be mindful of portion sizes. Eating large servings can lead to spikes in blood sugar levels. Using smaller plates and measuring food can help manage portions effectively.
Incorporate Fiber
Foods high in fiber, such as legumes, whole grains, fruits, and vegetables, can help regulate blood sugar levels. Fiber slows down digestion and helps maintain steady glucose levels.
Limit Refined Carbohydrates
Avoid foods high in refined carbohydrates, such as white bread, pastries, and sugary snacks. These can cause rapid increases in blood sugar. Opt for whole grain options instead, which are healthier and more filling.
Balance Your Plate
Each meal should include a balance of carbohydrates, proteins, and healthy fats. A well-balanced plate can help control blood sugar levels and keep you satisfied.
Stay Hydrated
Drinking enough water is vital for overall health. Staying hydrated can improve insulin sensitivity and help manage blood sugar levels. Aim for at least eight glasses of water a day.
Plan Meals Ahead
Planning meals in advance can help you make healthier choices. Consider preparing a meal plan for the week, focusing on nutritious foods and avoiding last-minute unhealthy options.
Seek Professional Guidance
Consulting with a registered dietitian can provide personalized advice tailored to your specific needs. They can help you create a customized meal plan that fits your lifestyle and health goals.
Importance of regular monitoring
Regular monitoring is crucial in managing diabetes effectively. Keeping track of blood sugar levels helps individuals understand how their body responds to different foods, activities, and medications. Here are some key points about the importance of regular monitoring:
Understanding Blood Sugar Patterns
By consistently checking blood sugar levels, individuals can identify patterns and understand how their diet, exercise, and stress levels impact their glucose. This information is essential for making informed decisions about treatment.
Preventing Complications
Regular monitoring helps in preventing complications associated with diabetes. High or low blood sugar levels can lead to severe health issues over time, including nerve damage, kidney problems, and heart disease. By keeping levels in check, individuals can reduce the risk of these complications.
Adjusting Treatment Plans
Monitoring allows for timely adjustments to treatment plans. If blood sugar levels are consistently high or low, it may indicate that changes are needed in medication, diet, or exercise routine. Working closely with healthcare providers ensures that adjustments are based on accurate data.
Promoting Accountability
Regular blood sugar checks can promote a sense of accountability in managing diabetes. By tracking results, individuals can stay motivated and committed to their health goals. This can be particularly helpful in maintaining a healthy lifestyle.
Empowering Individuals
Knowledge is power. Regular blood glucose monitoring empowers individuals by providing them with the information they need to take control of their diabetes. When they understand their readings, they can make better choices regarding their health.
Using Technology
Advancements in technology have made monitoring easier than ever. Continuous glucose monitors (CGMs) provide real-time data, while mobile apps can help track readings and analyze trends. These tools can enhance engagement in one’s health management.
When to seek medical help

Knowing when to seek medical help for diabetes is crucial for maintaining health and preventing complications. While regular check-ups are important, recognizing warning signs that require immediate attention can greatly improve outcomes. Here are key indicators that it’s time to consult a healthcare professional:
Symptoms of High Blood Sugar
If you experience persistent symptoms of high blood sugar, such as increased thirst, frequent urination, extreme hunger, or blurred vision, it’s important to seek medical advice. These signs indicate that your blood sugar may be too high and require adjustment in your management plan.
Symptoms of Low Blood Sugar
On the other hand, symptoms of low blood sugar can include sweating, shaking, confusion, and dizziness. If you notice these symptoms, checking your blood sugar level is essential. If it is low, consuming fast-acting carbohydrates is usually needed, but if symptoms continue, seek medical help.
Persistent Fatigue
Feeling constantly tired or exhausted can be a sign that diabetes is not well-managed. Consult your healthcare provider if you experience persistent fatigue that interferes with daily activities or does not improve with rest.
Infections or Wounds That Don’t Heal
People with diabetes are at a higher risk for infections. If you notice wounds or cuts that are slow to heal, or if you have persistent infections such as gum disease or skin infections, it’s crucial to seek medical attention.
Changes in Vision
Blurred vision or sudden changes in eyesight can indicate fluctuating blood sugar levels. It’s vital to see an eye specialist if you experience these symptoms, as they could lead to serious conditions like diabetic retinopathy.
Foot Problems
Diabetes can affect circulation and nerve function in the feet. If you experience numbness, tingling, or foot sores that do not heal, consult a healthcare professional to prevent complications like ulcers or infections.
Regular Health Check-ups
Even if you’re not experiencing symptoms, regular health check-ups are essential. These visits allow for monitoring of diabetes management, potential complications, and overall health. Discuss any concerns or changes in your health during these appointments.
Impact of stress on diabetes symptoms
Stress can significantly impact diabetes symptoms and management. Understanding the relationship between stress and blood sugar levels is essential for effective diabetes care. Here are key points to consider regarding the impact of stress on diabetes symptoms:
Stress Hormones and Blood Sugar
When a person is stressed, the body releases stress hormones like cortisol and adrenaline. These hormones can cause an increase in blood sugar levels, making diabetes management more challenging.
Physical Reactions to Stress
Stress triggers physical reactions in the body, such as increased heart rate and rapid breathing. These changes can lead to higher blood sugar levels, as the body prepares for a “fight or flight” response. If stress is chronic, this can lead to consistently elevated blood sugar levels.
Mood Changes and Food Choices
Stress often affects mood, which can lead to unhealthy food choices. Individuals may turn to comfort foods that are high in sugar and fat, which can negatively impact blood sugar control. Opting for healthier stress-relief methods can help maintain better blood sugar levels.
Impact on Routine
High stress can disrupt daily routines, making it difficult to stick to healthy habits. For example, stress might lead to skipping exercise or forgetting to take medications, both of which are vital for managing diabetes effectively.
Managing Stress Levels
Implementing stress management techniques is crucial. Practices such as mindfulness, meditation, deep breathing exercises, and regular physical activity can help reduce stress and improve blood sugar control.
Seeking Support
Talking about stress and its impact on diabetes with friends, family, or a mental health professional can provide support. Joining support groups can also introduce helpful strategies to cope with stress and maintain better health.
Recognizing Symptoms
Understanding how stress affects individual diabetes symptoms can improve management. Recognizing stress-related symptoms can help in taking proactive steps to alleviate stress and keep blood sugar levels stable.
How exercise benefits diabetes management

Regular exercise is a crucial component of diabetes management. Physical activity helps control blood sugar levels and brings many other health benefits that can improve quality of life. Here are some key ways exercise positively impacts diabetes management:
Improving Insulin Sensitivity
Exercise increases insulin sensitivity, which means that cells are better able to use available insulin to take up glucose from the bloodstream. This can lead to lower blood sugar levels and improved diabetes control.
Weight Management
Physical activity helps with weight management. Maintaining a healthy weight is vital for those with diabetes, as excess weight can contribute to insulin resistance. Regular exercise can help achieve and maintain a healthy body weight.
Lowering Blood Sugar Levels
During exercise, muscles use glucose for energy, which can lead to a decrease in blood sugar levels. This effect can last for hours or even days after exercising, providing an important benefit for blood sugar management.
Reducing Stress
Exercise is a powerful stress reliever. Physical activity reduces levels of stress hormones in the body and releases endorphins, which improve mood. Managing stress is important for diabetes control, as stress can negatively affect blood sugar levels.
Improving Heart Health
People with diabetes are at an increased risk for heart disease. Regular exercise strengthens the heart and improves circulation. This can lower the risk of heart-related complications and promote better overall health.
Boosting Energy Levels
Engaging in regular physical activity can boost energy levels and enhance overall well-being. Improved energy can make it easier to maintain a healthy lifestyle and adhere to diabetes management routines.
Building a Support System
Exercise can also create opportunities to connect with others. Joining group classes or clubs can foster a sense of community and support, helping you stay motivated and accountable to your fitness goals.
Myths about diabetes symptoms
There are many myths surrounding diabetes symptoms that can lead to misunderstanding about the condition. Dispelling these myths is essential for awareness and effective management. Here are some common misconceptions:
Myth 1: Diabetes Only Affects Overweight People
This myth is not true. While being overweight can increase the risk of developing type 2 diabetes, people of all body types can develop diabetes, including those who are thin or of average weight. Genetic factors and lifestyle choices also play a significant role.
Myth 2: Only Older Adults Get Diabetes
Another misconception is that diabetes only affects older adults. In reality, type 1 diabetes often appears in childhood or adolescence, while type 2 diabetes is increasingly being diagnosed in younger populations due to rising obesity rates and sedentary lifestyles.
Myth 3: People with Diabetes Can’t Eat Sugar
While those with diabetes need to monitor their sugar intake, they do not need to completely avoid sugar. It’s important to maintain a balanced diet, and moderation is key. People with diabetes can include small amounts of sugar in their meal plans.
Myth 4: Diabetes Symptoms Are Obvious
Many believe that the symptoms of diabetes are always obvious, such as extreme thirst or frequent urination. However, early symptoms can be subtle and may go unnoticed. Regular check-ups and blood tests are crucial for early diagnosis.
Myth 5: Insulin Is Only for Severe Cases of Diabetes
This belief is incorrect. Insulin therapy is necessary for many people with type 1 diabetes from the start. Some individuals with type 2 diabetes may also require insulin as their condition progresses to maintain proper blood sugar levels.
Myth 6: If You Have Diabetes, You Will Experience Symptoms All the Time
Diabetes symptoms can vary from person to person and can change over time. Some may not experience noticeable symptoms at all. Regular monitoring is essential to manage the condition effectively, even if a person feels fine.
Myth 7: Diabetes Is Not a Serious Disease
Diabetes is a serious condition that can lead to complications if not managed properly. Misunderstanding the risks associated with diabetes can prevent individuals from seeking necessary care and making lifestyle changes.
Long-term complications of uncontrolled diabetes
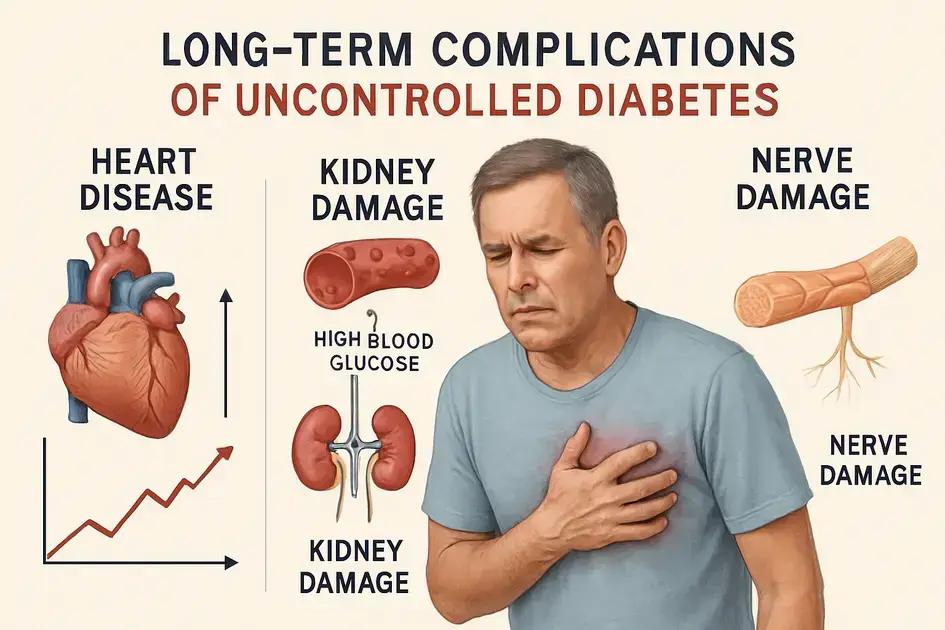
Uncontrolled diabetes can lead to several serious long-term complications that affect various systems in the body. Managing diabetes effectively is crucial to prevent these complications and maintain overall health. Here are some significant long-term effects of unchecked diabetes:
Cardiovascular Disease
People with uncontrolled diabetes are at a higher risk for cardiovascular disease. This includes conditions such as heart attacks, strokes, and high blood pressure. Diabetes can damage blood vessels and nerves that control the heart and blood vessels.
Kidney Damage
Diabetes can lead to a condition known as diabetic nephropathy, which affects the kidneys’ ability to filter waste from the blood. Over time, this can result in kidney failure, necessitating dialysis or a kidney transplant.
Nerve Damage (Neuropathy)
High blood sugar levels can cause nerve damage. This condition, known as diabetic neuropathy, can result in symptoms such as pain, tingling, and numbness, particularly in the feet and hands. It can also affect digestion and sexual health.
Eye Problems
Uncontrolled diabetes increases the risk of serious eye conditions, including diabetic retinopathy, which can lead to blindness. Other issues include cataracts and glaucoma, highlighting the need for regular eye exams.
Foot Complications
Diabetes can cause poor blood flow and nerve damage in the feet, leading to foot complications. This includes infections, ulcers, and in severe cases, amputations. Proper foot care and regular check-ups are vital for prevention.
Skin Conditions
People with diabetes may experience a variety of skin conditions, including bacterial and fungal infections. High blood sugar levels can also lead to dry skin and increased risk of skin disorders.
Impact on Mental Health
Living with diabetes and its complications can lead to feelings of depression and anxiety. Mental health support is crucial for emotionally coping with the challenges of managing diabetes.
Patient stories: living with diabetes
Sharing patient stories can offer valuable insights into the daily lives of individuals living with diabetes. These personal experiences highlight the challenges, triumphs, and lessons learned along the way. Here are some impactful narratives of people managing their diabetes:
Maria’s Journey with Type 1 Diabetes
Maria was diagnosed with type 1 diabetes at the age of 10. She shares how she learned to manage her condition by monitoring her blood sugar levels and administering insulin regularly. Maria emphasizes the importance of family support and how her parents helped her understand the need for a balanced diet and regular exercise. Her story inspires others by showing that, with determination, it’s possible to lead a full and active life.
John’s Experience with Type 2 Diabetes
John’s journey started when he was diagnosed with type 2 diabetes in his 40s. Initially, he struggled with lifestyle changes. However, after joining a local support group, he found motivation to eat healthier and exercise regularly. John’s story reflects the importance of community support. He now shares his experience to help others avoid the pitfalls he faced, emphasizing that it’s never too late to make positive changes.
Emily’s Story of Pregnancy with Gestational Diabetes
Emily faced a unique challenge when she was diagnosed with gestational diabetes during her pregnancy. She describes how she worked closely with her healthcare team to keep her blood sugar levels stable while ensuring the health of her baby. Through meal planning and routine exercise, Emily learned to manage her condition effectively. Her story highlights the importance of regular check-ups and staying informed during pregnancy.
David’s Proactive Approach
David has been living with diabetes for over 20 years. He advocates for self-management and regularly shares tips on how to keep blood sugar levels in check. His proactive approach includes staying updated with the latest diabetes technology, like continuous glucose monitors. David’s story is a testament to the power of knowledge and adaptation.
Lisa’s Emotional Journey
Living with diabetes can take an emotional toll. Lisa shares her struggles with anxiety and depression related to her diabetes management. She emphasizes the importance of mental health support and finding ways to cope with the emotional aspects of living with diabetes. Lisa’s story serves as a reminder that it’s essential to care for mental health as well as physical health in diabetes management.
Living with Diabetes: A Journey Toward Better Health
Managing diabetes is a continuous journey that involves understanding symptoms, making informed lifestyle choices, and seeking support when needed. Through the stories of individuals living with diabetes, we see the power of community, knowledge, and personal perseverance.
By addressing misconceptions, incorporating healthy habits, and remaining vigilant about monitoring health, those affected by diabetes can lead rich, fulfilling lives. Each person’s experience adds to the understanding of what it means to live with diabetes and highlights the importance of education and support in managing this condition.
Always remember, whether through exercise, proper diet, or emotional support, there is a path to better health for everyone living with diabetes.
FAQ – Frequently Asked Questions About Living with Diabetes
What are the common symptoms of diabetes?
Common symptoms of diabetes include increased thirst, frequent urination, extreme hunger, fatigue, and blurred vision.
How can I manage my diabetes effectively?
Effective diabetes management includes monitoring blood sugar levels, maintaining a balanced diet, exercising regularly, and adhering to medication schedules.
What should I do if I experience symptoms of high or low blood sugar?
If you experience symptoms of high blood sugar, such as excessive thirst or fatigue, contact your healthcare provider. For low blood sugar, consume fast-acting carbohydrates and monitor your levels closely.
Are there support groups for people living with diabetes?
Yes, there are many support groups available, both in-person and online, where individuals can share experiences, advice, and encouragement with others living with diabetes.
What role does exercise play in diabetes management?
Regular exercise helps improve insulin sensitivity, manage weight, lower blood sugar levels, and reduce stress, all of which are important for effective diabetes management.
How can I prevent long-term complications from diabetes?
To prevent long-term complications, it is vital to keep blood sugar levels within the target range, eat a balanced diet, exercise regularly, and have regular check-ups with your healthcare provider.








